2800 Valmont Road
Boulder, CO 80301
Boulder, CO 80301
- Phone: (303) 443-2257
- Fax: (303) 443-4599
- Monday: 10:00 AM - 6:15 PM
- Tuesday: 10:00 AM - 6:15 PM
- Wednesday: 10:00 AM - 6:15 PM
- Thursday: 10:00 AM - 6:15 PM
- Friday: By Appointment Only
- Saturday: 10:00 AM - 4:00 PM
- Sunday: Closed
Optometrists Change Lives by the Optometric Extension Program Foundation: www.oepf.org

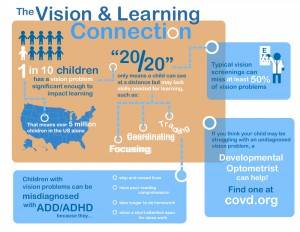
Infographics by the College of Optometrists in Vision Development. For more information visit: www.covd.org


Notes:
Please contact us with any questions you might have at bouldervt@yahoo.com.